What Is Central Sensitization? Does It Impact Procedures?
Credit: Shutterstock
Central Sensitization is such a critical concept for some patients with chronic pain that it’s just begging for me to cover it, so here goes. So what is Central Sensitization? Why is it important? If you have it, how should you navigate procedures? Let’s dig in.
What is Central Sensitization?
When you feel pain, those signals are carried by nerves. Hence, nerves are a key part of your perception of pain. Another key part is your brain that registers the signal. Your sympathetic and other parts of your nervous system spend quite a bit of time regulating your pain and helping you ignore it. For example, we’ve all experienced having something that hurts, but when you’re focusing your attention elsewhere, you don’t notice it. That’s because your body has inhibitory circuitry that can temporarily inhibit the pain signal.
What if we took all of the brakes off the pain and made the nerves very efficient at carrying pain signals? That’s called Central Sensitization (CS). Meaning small things cause big pain.
Temporal Summation and Wind Up
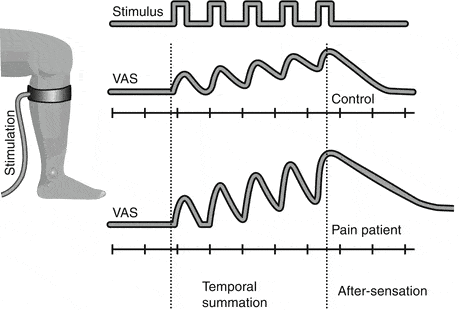
Temporal summation means that pain signals get added together rather than happening as individual events that each die off. If you look above, a pain stimulus in the form of a blood pressure cuff is used on a leg. In the normal patient, while there is some additive pain effect (building of the height of the VAS pain score) by repeatedly blowing up the cuff, that pales in comparison to what happens in the patient with CS on the bottom. In that case, the pain builds sharply as the number of cycles increases. That’s also called “wind-up”.
This phenomenon can be seen in CS patients who get procedures. Meaning that while injecting a bunch of different body sites for a normal patient might cause each of those several sites to hurt a little bit, in the CS patient, these sites all add together to make the overall experience of pain much higher than it should be.
Something else to be aware of is that in some CS patients, the areas of pain hypersensitivity often don’t follow single nerve pathways but tend to be more regional. Rarely, this can evolve into Complex Regional Pain Syndrome where even movement or light touch can be painful. CRPS is like CS on steroids.
What Causes Central Sensitization?
One of the traditional models for CS is similar to CRPS. This is believed to be a problem with the system that provides the brakes for pain signals. Another possibility is an injury to key nerves or the spinal cord. One of the newer theories for why CS happens is neuroinflammation (2). This is inflammation that impacts nerves which can happen if the patient has high total body inflammation. Also, metabolic syndromes (overweight, high blood pressure, low activity) can cause or make this problem worse.
How Do You Know if You Have This Problem?
Again, patients with CS have pain that’s intense and out of proportion to the tissue damage (1). It also lasts way longer than one would normally expect. Here are some things that many patients with central sensitization report:
- Things like a massage can cause increased pain for days to weeks
- Acupuncture or injections can cause a similar or worse flare-up
- Surgery can result in months of severely increased pain
Realize that a small handful CS patients can even experience a quasi-permanent increase in pain from a procedure where pain can be increased for months to years. However, that’s very rare. More common is to take whatever the normal recovery time should be and multiply it by 3-20X.
Rules for CS Patients and Procedures
After treating hundreds of patients over the past few decades who have CS, there are a couple of helpful tips for how to get these patients to be able to better tolerate injection procedures.
Less is More
One of the things you can do to help reduce procedure-related flare-ups of CS is to get fewer pokes. For example, you may want to get it all done at once, but less is more. So if 5 injections were planned for the neck, and 10 for the shoulder, and 5 for the knee for a total of 20 sites, reducing that to 5 injections will often help limit the flare-up.
Anesthesia
One of the keys for CS patients is to make sure they are asleep during procedures. This reduces the up-regulation of the area and reduces recovery time. Hence, being “knocked out” with an IV (Total IV Access Anesthesia) during the procedure is often important.
Any Meds that Help?
One of the most reliable medications that help CS patients I have ever seen is Lyrica (pregabalin). While many patients get placed on Neurontin (gabapentin), this is much less effective in our experience. Lyrica is usually started at night for a few weeks until the patient gets used to it and then a morning dose is added in.
Can CS Be Treated?
The short answer is yes. In my experience, helping the individual pain areas that started the bonfire can mean that the CS improves. In patients who have failed conservative care like physical therapy, acupuncture, and/or chiropractic, this is often accomplished by an orthobiologic injection. This is why being able to successfully inject these patients is critical.
Summary
Central Sensitization means that the normal brakes on pain have been removed. Pain signals are therefore amplified. Procedural-based care can be a two-edged sword, it can both help (if done carefully) or make the patient worse. Hence, the concept that less procedural care is more can make a big difference. Anesthesia and meds can also assist in navigating the CS minefield.
The upshot? If you have an exaggerated pain response to things like a massage or an injection, you may have central sensitization. If you do, there are some rules to help you tolerate procedures.
__________________________________
References:
(1) Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain. 2011;152(3 Suppl):S2-S15. doi:10.1016/j.pain.2010.09.030
(2) Ji RR, Nackley A, Huh Y, Terrando N, Maixner W. Neuroinflammation and Central Sensitization in Chronic and Widespread Pain. Anesthesiology. 2018;129(2):343-366. doi:10.1097/ALN.0000000000002130

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
