Knee Stem Cell Injections for Arthritis: Do Stem Cells Help People with Severe Arthritis – An Analysis of our Published Data…
We have ample evidence that knee stem cell injections for arthritis work. Do we have evidence that cultured knee stem cell injections can work for severe knee arthritis? This morning I’d like to review our registry data on how patients with different levels of arthritis responded to the Regenexx-C procedure. This is the procedure that is only offered down in the Cayman islands.
First, as of this morning, indexed in the U.S. National Library of Medicine there are 2,257 indexed articles on mesenchymal stem cells and cartilage, 430 on these cells and arthritis, and 23,600 on just this one stem cell type. Let’s vet the issue of whether a cultured stem cell treatment may be effective for a patient with severe arthritis and if so, how would that work. In fact, to better explore how our published research fits on this topic, let’s delve a bit further into that paper and other data from that same data-set.[1]
In our research, 67.8% of patients were total knee arthroplasty candidates at the time of first treatment. Despite this, only 6.9% of the treated knee patients reported that they had opted for knee replacement despite MSC treatment. What does this mean? It means that 2/3’rds of the patients in this study were “bone on bone” when we began to treat them. Despite that, only about 7% of the treated patients felt the need to get a knee replacement during the study.
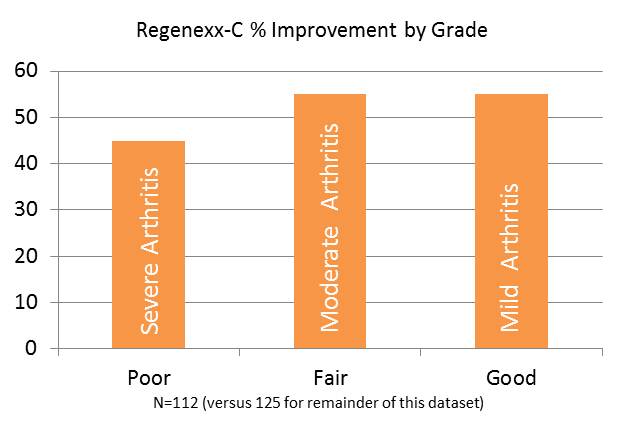
The graph above is also helpful to explain these issues. This is found on the RegenexxCayman web-site (www.regenexxcayman.ky). This is another slice of the same data-set, this time the data is broken out by severity of arthritis. This is the mean improvement (read average improvement) by the degree of arthritis. The numbers on the y-axis of the graph that span from 0-60 correspond with the average percentage improvement by all patients in that category. Note that in these 112 patients, there isn’t a huge difference in average reported outcome by severity grade. The patients with mild and moderate arthritis have done only marginally better than those with severe arthritis.
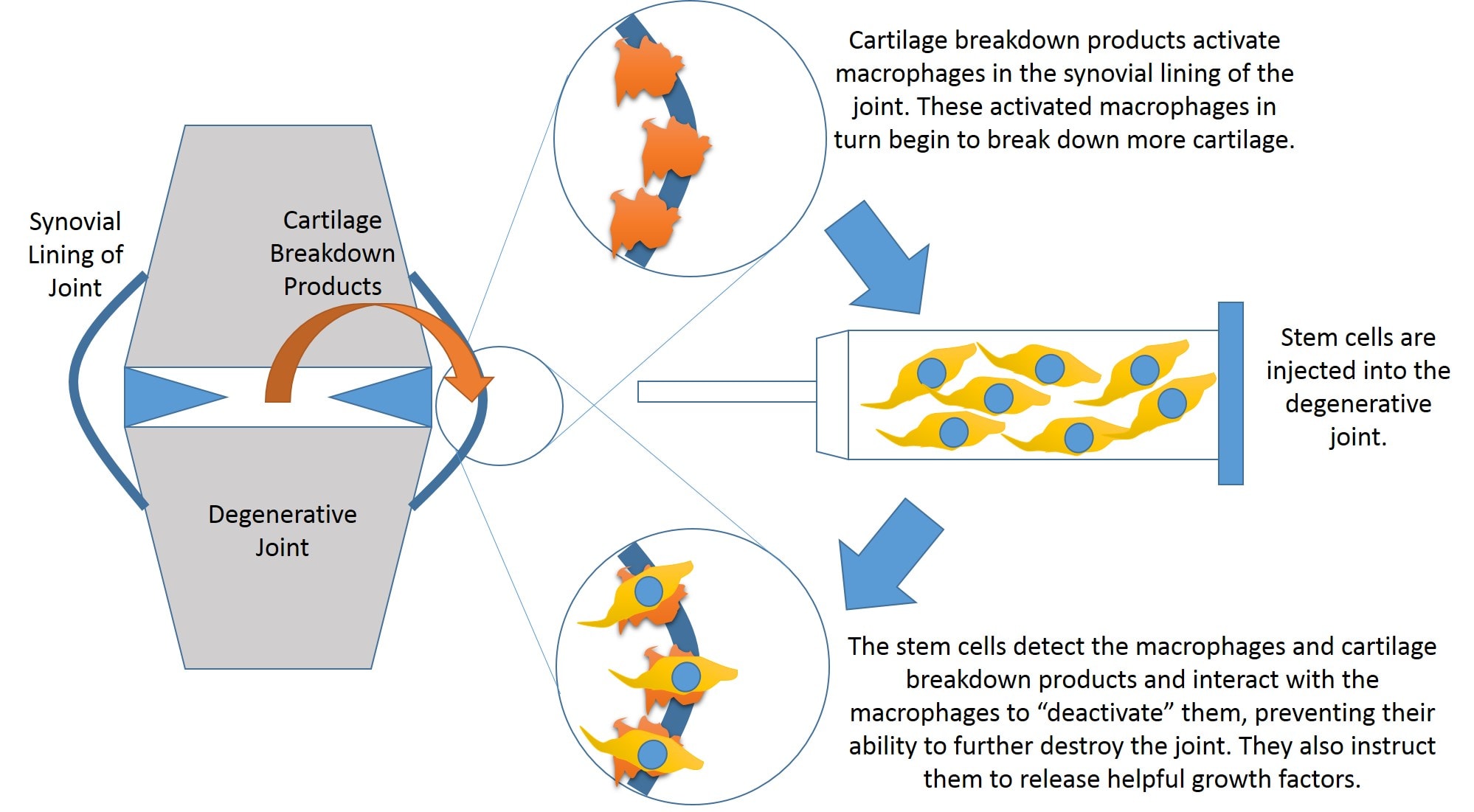
Does this involve regrowing large swaths of cartilage? No, our pre and post MRIs haven’t shown that in patients with severe arthritis. How would this work then? One recent study is illustrative.[2] I’ve taken these rather difficult to understand jargon laden concepts and created an illustration (below) to make them simpler to understand. In a degenerating joint with severe arthritis, the lining of the joint (called the synovial lining) becomes thickened with macrophages. These cells are like big pac man cells that eat the cellular debris and help clean up the garbage in the joint. The problem with arthritis is that all the debris causes these pac men to become more activated so that they eventually begin gobbling up even some of the good joint cartilage. This causes more damage in a positive feedback loop. This research team found that in a model of severe arthritis, stem cells injected into the joint detected the activated macrophages and deactivated them, allowing the pac man function to be turned off. In addition, the stem cells instructed the bad macrophages to secrete good growth factors, essentially turning them from destroyers to helpers. They believe this explains the long-term anti-inflammatory effect seen with stem cells. Others have come up with other mechanisms.
What’s the evidence that a knee replacement will help a knee with severe arthritis? A recent study questions the efficacy of knee replacement.[3] Out of about 130 patients undergoing a knee replacement, only 53.5% experienced a good outcome. A study last year in the Lancet by Carr is also helpful to understand what we know and don’t know about knee replacement outcomes.[4] From the Medpage Today article quoting the study author:
“Long-term data on total knee replacement surgery is largely limited to revision, leaving clinicians and patients in the dark about outcomes such as residual pain and disability, researchers said.
Currently the best data come from national procedure registries, but the traditional outcome measure is subsequent revision surgery, which “can underestimate problems [because] patients can remain with pain or poor function without necessarily undergoing revision,” according to Andrew J. Carr, FMedSci, of the University of Oxford in England, and colleagues.”
Another study last year found significant issues with a lack of return to normal expected activities after knee replacement.[5] In this study patients were able to exercise only about half as much as they had planned prior to the knee replacement. Finally, yet another recent study found that patients with the most severe arthritis didn’t have significant improvements in pain and function after knee replacement.[6]
What are the risks of knee replacement? Quite significant. Based on our review of the National Inpatient Sample Database, in knee replacement patients in 2008 (only Medicare) there were an estimated 4,964 deaths, 2,788 pulmonary emboli, 2,908 myocardial infarcts, and 4,670 cases of pneumonia coded as being caused by the surgery.[1] Based on more recent research, we know that knee replacement surgery dramatically increases heart attack risk, with a 3,100% increase in heart attack risk in the two weeks after surgery.[7] In our 2011 paper, based on the ability to save some patients from needing a knee replacement surgery, we stated the following:
In our knee group, approximately 2/3rd’s were candidates for a knee arthroplasty and approximately 2/3rd’s reported a >50% reduction in symptoms at an average of just over 11 months post procedure. Over the complications observation period, only 6.9% of the treated knee patients reported that they had opted for knee replacement despite MSC treatment. A recent retrospective study of more than 17,000 total knee arthroplasties (TKA) demonstrated that serious surgical complications were quantifiable [33]. Applying these surgical complication rates to our 374 knee procedures discussed in this paper would yield the following complications:
1. 29-37 patients with serious surgical complications.
2. Approximately 1-2 mortalities as a result of the procedure.
3. Approximately 2 patients with pulmonary emboli.
4. Approximately 2-16 patients with a hospital
Meaning that if the patients in our research study undergone a knee replacement instead of a stem cell injection, almost 40 would have serious complications and 1-2 of them would have died of complications from the knee replacement. No such complications were seen in our study.
In conclusion, since 2005 we have published a good deal of the human stem cell research in orthopedic injuries that exists in the US National Library of Medicine and in other peer reviewed journals.[8-13] [also see https://regenexx.com/results/research/]. I have also authored two book chapters on the use of stem cells in orthopedic injuries. We now have the largest clinical registry of orthopedic stem cell treated patients in the world with more than 2,000 patients. All of this has taught us that a reasonable number of patients with severe arthritis do respond to a cultured stem cell procedure.
The above data is based on a registry trial with a comparison group (data collected while patients treated) and is not based on a randomized controlled trial. RegenexxCayman is an independently owned and operated medical services provider operating exclusively in the Cayman Islands and is not part of or affiliated with the Centeno-Schultz Clinic or any U.S. Regenexx Network provider. The Regenexx-C procedure licensed by RegenexxCayman is not approved by the U.S. FDA for use in the United States.
1. Centeno, C.J., et al., Safety and complications reporting update on the re-implantation of culture-expanded mesenchymal stem cells using autologous platelet lysate technique. Curr Stem Cell Res Ther, 2011. 6(4): p. 368-78.
2. van Lent, P.L. and W.B. van den Berg, Mesenchymal stem cell therapy in osteoarthritis: advanced tissue repair or intervention with smouldering synovial activation? Arthritis Res Ther, 2013. 15(2): p. 112.
3. Hawker, G.A., et al., Which patients are most likely to benefit from total joint arthroplasty? Arthritis Rheum, 2013. 65(5): p. 1243-52.
4. Carr, A.J., et al., Knee replacement. Lancet, 2012. 379(9823): p. 1331-40.
5. Jones, D.L., et al., Differences between actual and expected leisure activities after total knee arthroplasty for osteoarthritis. J Arthroplasty, 2012. 27(7): p. 1289-96.
6. Shearer, D.W., et al., The predictors of outcome in total knee arthroplasty for post-traumatic arthritis. Knee, 2013.
7. Lalmohamed, A., et al., Timing of acute myocardial infarction in patients undergoing total hip or knee replacement: a nationwide cohort study. Arch Intern Med, 2012. 172(16): p. 1229-35.
8. Carpenter, R.S., et al., Osteoblastic differentiation of human and equine adult bone marrow-derived mesenchymal stem cells when BMP-2 or BMP-7 homodimer genetic modification is compared to BMP-2/7 heterodimer genetic modification in the presence and absence of dexamethasone. J Orthop Res, 2010. 28(10): p. 1330-7.
9. Centeno, C.J., et al., Increased knee cartilage volume in degenerative joint disease using percutaneously implanted, autologous mesenchymal stem cells. Pain Physician, 2008. 11(3): p. 343-53.
10. Centeno, C.J., et al., Partial regeneration of the human hip via autologous bone marrow nucleated cell transfer: A case study. Pain Physician, 2006. 9(3): p. 253-6.
11. Centeno, C.J., et al., Safety and Complications Reporting on the Re-implantation of Culture-Expanded Mesenchymal Stem Cells using Autologous Platelet Lysate Technique. Curr Stem Cell Res Ther, 2009.
12. Barallobre-Barreiro, J., et al., Comparison of gene expression profiles in a porcine infarct model after intracoronary, transthoracic, or transendocardiac injection of heterologous bone marrow mesenchymal cells. Transplant Proc, 2009. 41(6): p. 2279-81.
13. Centeno, C.J., et al., Regeneration of meniscus cartilage in a knee treated with percutaneously implanted autologous mesenchymal stem cells. Med Hypotheses, 2008. 71(6): p. 900-8.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.