Why Interventional Orthopedics Is the Disruptive Tech We All Need
Surgical orthopedics is irreparably broken. High-level study after high-level study has been published this past decade showing that the surgical procedures we all believed were highly effective, like arthroscopic knee surgery, are no better than sham or placebo surgery. This is why the time is ripe to replace much of surgical orthopedics with a new medical specialty requiring new skills, tools, and knowledge—interventional orthopedics. Let me explain.
How Broken Is Surgical Orthopedics?
Ever since the invention of the arthroscope and its wider use in the 1980s, surgical orthopedics has dominated musculoskeletal care. The reason was that surgeons suddenly had a way to perform their craft through a smaller incision, and they could “see” what was wrong as they “fixed it.” Seeing and fixing is a powerful concept, so the idea caught on like wildfire.
Most people don’t realize that surgical orthopedics began its long steady decline with its naked in Times Square moment in 2002 when a single research paper changed everything. The Moseley study was the first large-scale randomized controlled trial to be performed on a very common orthopedic surgical procedure. At the time, a good portion of patients with painful arthritic knees underwent arthroscopic debridement surgery. Basically, the surgeon poked the scope in and looked around and saw a “dirty room” with pieces of cartilage floating around, frayed and torn meniscus parts, and holes in the cartilage surfaces. The surgeon would then “clean up” the area by snipping and tucking and shaving and then wash the whole thing out. Billions were spent annually on these surgeries. That was until Moseley showed that it was all no better than an elaborate hoax, as the procedure didn’t perform any better than a series of faked surgeries he and his team had performed.
If Moseley marked the beginning of the high water, the flood was soon to follow. In recent years additional high-level studies have debunked all types of meniscus surgery for any indication as well as most rotator cuff surgeries. Low back fusion surgery after a laminectomy is the most recent victim of a deluge of research showing that traditional arthroscopic or spine surgery is ineffective. This is despite hundreds of billions in annual spending. In addition, we also have no high-level research on the effectiveness of common procedures, such as hip arthoscopy, so expect more surgical sacred cows to be felled in the next decade.
Why Is This Happening?
The idea that structure equals function is a powerful one. We all believe that the little spot we see on an MRI is surely the cause of our pain, but research has shown that this is often not the case. In fact, it’s clear that we’re often operating on phantoms, as just as many patients without pain have the same MRI abnormalities. In addition, another problem facing surgical orthopedics is that it can be like a bull in the proverbial china shop. Much damage can be done just getting to tissues, despite the fact that arthroscopic procedures are called “minimally invasive.” As an example, most patients don’t know that routine arthroscopic hip surgery involves putting so much traction on the hip that one of the main nerves of the leg loses its ability to conduct signals during the surgery and must be monitored to prevent nerve damage.
Interventional Orthopedics to the Rescue
Interventional orthopedics means using precise imaging-guided procedures to place things that can heal tissues in specific areas of need. To figure out what interventional orthopedics (IO) is, it’s first helpful to look at what it’s not:
- A surgeon using a blind knee injection or using ultrasound to make sure he or she is performing a simple platelet rich plasma joint injection is not IO.
- A doctor performing a simple hip injection of stem cells into the joint using ultrasound is also not IO.
Let me explain. This past week I reviewed the credentials of a physician who wanted to apply for our mini-fellowship, which is three months of training in interventional orthopedics. Because that training is intensive, the physician needed to be better trained than 90% of the doctors in his specialty of PMR in both advanced, precise guided spinal injections and have some experience with ultrasound-guided joint injections. Like 90% of the doctors I have considered for this fellowship, this doctor was turned down due to a lack of basic interventional orthopedics training.
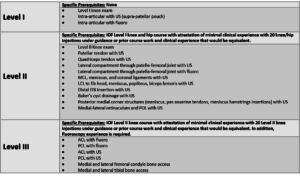

So it’s clear that if the future of precise IO is to take hold and we can all have access to high-quality, precise injection procedures, we need to retrain a nation of physicians. What you see here at the Regenexx website is the beginning of that disruptive technology. We handpick and then extensively train our physicians and certify them in specific body areas. No one else offering stem cells and/or PRP does that. In fact, >95% of the doctors offering these procedures right now for knee, hip, and shoulder issues wouldn’t qualify to be included in our physician network or for a three-month mini-fellowship.
What’s even more remarkable than our dedication to high-quality, precise imaging-guided interventional orthopedics is that we want the huge gap between where we’re practicing and where everyone else is practicing to be closed. To that end, we helped found the Interventional Orthopedics Foundation (IOF) and have made sure that this organization can follow its own path independent of Regenexx. To that end IOF is pursuing a goal of intensive education to get other physicians up to our level. Why support training your competition? Because it’s what benefits society the most.
Where Is IO Headed?
Our goal for IO is to compete head-to-head with surgical orthopedics, because when a disruptive technology competes with an established one, everybody benefits. In many areas, we believe IO will win out because it’s less invasive and will be able to offer better outcomes with less recovery time. In some areas surgery will remain the standard.
In the future expect the sophistication of IO to grow to unimaginable levels. For example, who would have foreseen that the cardiologists of the 1980s who could only prescribe meds, read an EKG, and perform a stress test would be the disruptive innovators of the 21st century? Interventional cardiology has largely replaced most of cardiothoracic surgery. Interventional cardiologists can now even replace valves by inserting specialized devices through the skin! IO will similarly soon be able to approximate retracted and torn tendons and ligaments without surgery, reshape abnormal bones through a needle, and routinely fix tissues with only a precise injection. Don’t believe this is possible? Read on.
The upshot? Regenexx is more than magic stem cells as the Internet is full of magic stem cell pixie dust. Regenexx is advanced interventional orthopedics that your surgeon or doc down the street who performs ultrasound-guided knee injections or fluoroscopy-guided spine injections can’t yet replicate. Interventional orthopedics is the technology that will disrupt surgical orthopedics and make musculoskeletal care better. It’s the future that consists of more than just sprinkling magic stem cells into existing broken surgeries; it’s reinventing how to fix problems like arthritic knees, torn menisci, ACLs, and rotator cuff tendons. If you’re a patient, dig deep into our website to lean more. If you’re a physician, welcome to the future. IOF can help you catch up to the industry leaders.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.