Orthopedic Surgery vs PRP and the Double Standard in Orthobiologics
Orthopedic surgery has one of the poorest evidence bases of any medical specialty. That’s not my opinion, but that of an academic writing in the British Medical Journal. Interventional Orthobiologics as a field, while new, has pretty solid and evolving evidence. However, both insurers and surgeons often complain that we need more orthobiologics research while ignoring the poor research support for orthopedic surgery, What gives? Let’s dig in.
Scandalously Poor
In 2015, an academic researcher, published an editorial in the British medical Journal about the fact that about 80% of orthopedic sports medicine didn’t have high quality research to support that it worked. He used the very British phrase “scandalously poor” to describe orthopedic research and lamented that the field had one of the poorest evidence bases of any medical specialty. Why?
Placebo vs Sham
You’ve likely heard the term “placebo”. It means using a sugar pill in a drug study to reduce the likelihood of the “placebo effect”. That means that the patient reports improvement in their condition not because of the treatment, but because of their beliefs about the treatment. The problem with orthopedic surgery is that it has a massive placebo effect. Meaning we have a whole team of people who have gathered to help the patient, incisions, anesthesia, braces, crutches and other things that cause patients to believe that they will be healed.
This surgical placebo effect is well documented. In fact, a 2014 study that reviewed 53 research articles found that 74% of time, the research on fake surgery showed a significant placebo effect. In a massive 51% of those studies, the surgery didn’t beat the placebo operation! (2) How’s that for a placebo!
When a surgical placebo procedure is used, it’s called a “sham”. This means that a fake procedure is performed by the doctor where the patient is opened up and closed without any other surgery being performed. Why are sham studies critical in orthopedics? Well, a 2017 study found that in all 6 sham studies testing orthopedic surgery they reviewed, the sham procedure was as good as the surgery for reducing pain and improving disability! (3)
How Have Common Orthopedic Surgeries Performed Against Sham So Far?
As noted above, we actually only have a handful of orthopedic surgeries that have been tested using a sham control, That means that the patients were randomized to get either the real orthopedic surgery versus the sham procedure. One of the earliest was arthroscopic debridement to treat knee arthritis and this research showed that the procedure didn’t work (4). Then came several studies on the very common procedure called partial menisectomy, which is performed when patients have knee meniscus tears. Again, this surgery didn’t work either (5).
Where Are the Surgical Sham Studies?
To get a sense of how many surgical studies use a sham control, I searched the US library of medicine for research on surgical rotator cuff repair. This procedure constitutes about a half million US surgeries and 2-5 billion USD a year in healthcare spending. Hence, it’s one of the most common orthopedic procedures offered to patients.
So what do we know about this procedure? There’s research showing that patients who opt for rotator cuff repair fair no better than someone who doesn’t get the surgery (6). We also know that when patients report that they’re improved, that this isn’t correlated with healing of their tear on MRI (which is the goal of the surgery), but instead levels of inflammatory chemicals in the joint (7). Finally, we also know that in one study, surgery couldn’t beat physical therapy (8). Hence, there are significant questions about whether this procedure works.
Despite studies questioning whether rotator cuff repair is effective, I was unable to find a single study where a placebo procedure (sham) was used. Think about that for a second. While we know this procedure is not highly effective, insurers are spending billions each year covering it, and yet we don’t have a single study comparing it to a sham operation.
Most all of the other common surgical procedures I researched also failed to have this gold standard research. There were RCTs, but almost all of these were comparing one surgical procedure to another, meaning the foundation studies comparing the surgery to sham/placebo were absent. This is bizarre in that we’re sitting here at the end of the second decade of the 21st century and most of the basic foundational research that supports that orthopedic surgery is effective is absent. Even more bizarre is that insurers are spending at least a hundred billion each year on these procedures.
Interventional Orthobiologics Research-PRP
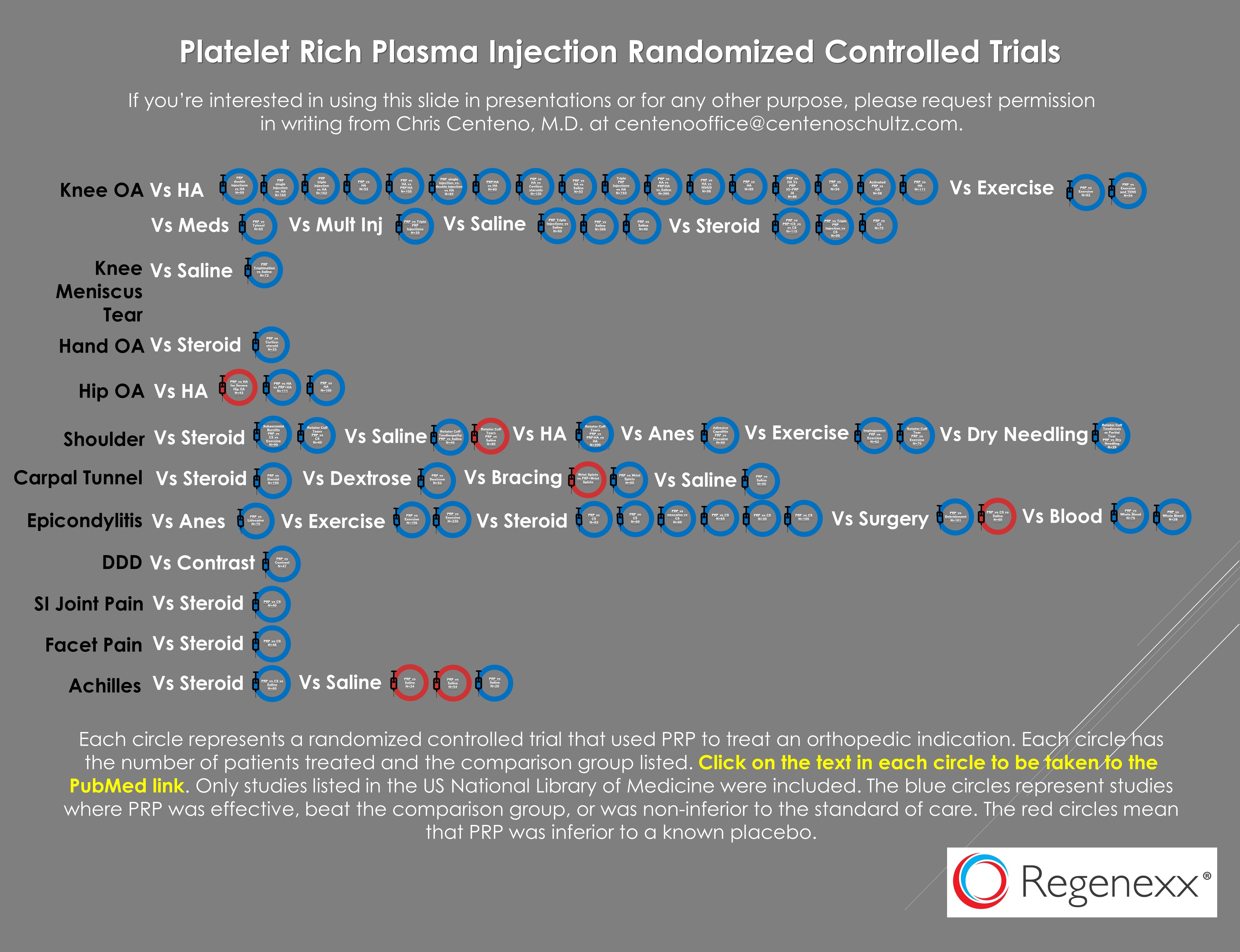
I recently performed a literature review on PRP injections to treat common musculoskeletal conditions. After all, about 80% of what I use all day to treat my patients are platelet based therapies, so that’s consistent with how I practice. Here’s what I found (click on the picture to be taken to a PDF with active links):
There were 66 randomized controlled trials as of last month. 12 of those were against what would be considered a placebo control and the remainder were compared to what would be considered the conservative standard of care. 60 of these studies showed positive results. So why in the world would any insurer not cover PRP when they already cover surgeries that have less research?
Comparing Surgery Research to PRP
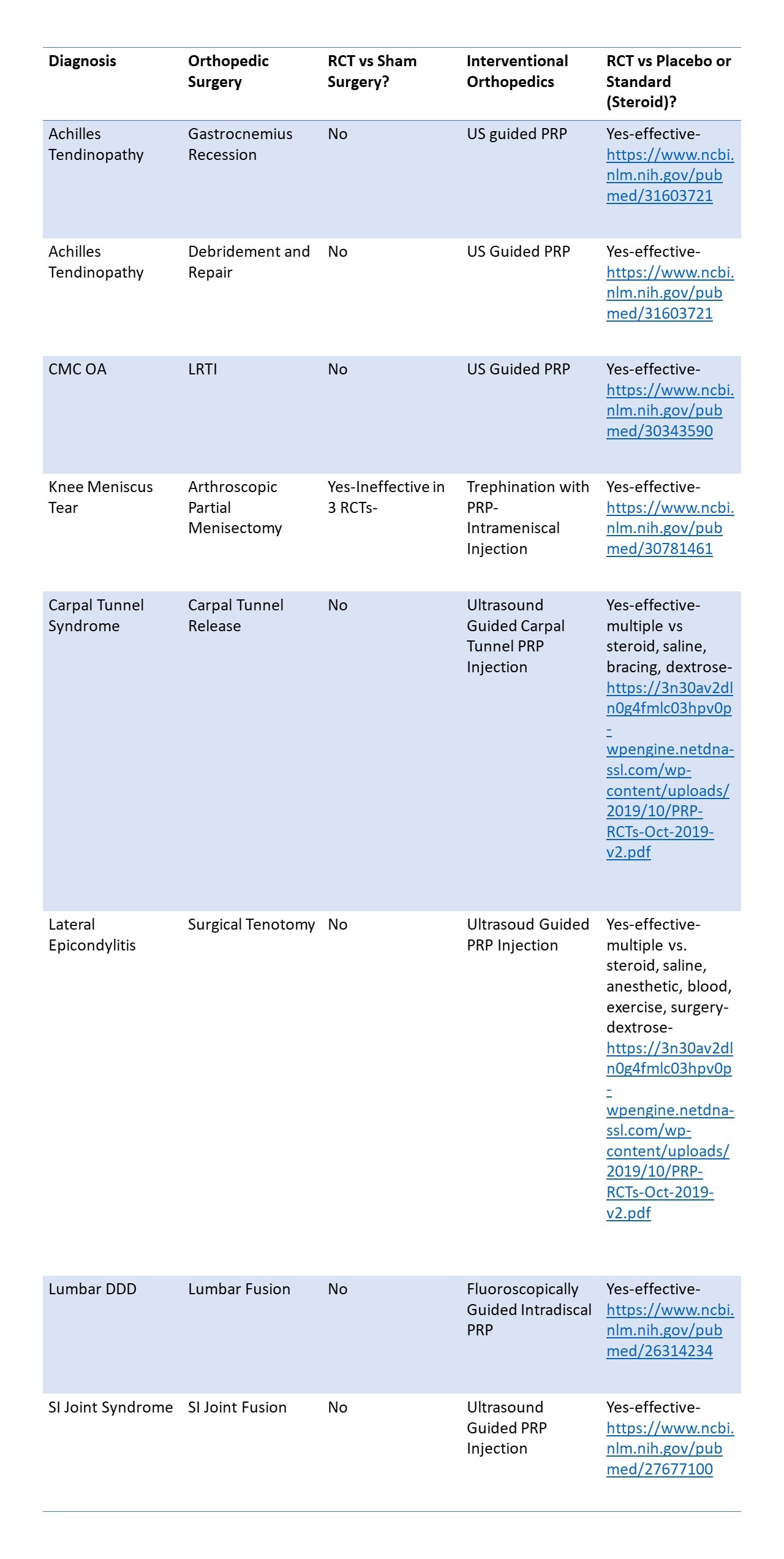
OK, now let’s compare some surgical procedures on whether sham studies are published and how that compares to PRP injections who have either placebo or conservative standard of care RCTs (click on the document to be taken to a PDF with active links):
So what do we see? For most of these common orthopedic procedures, no high-level foundational studies exist. As you can see, for PRP, the RCTs are there. So why again are insurers covering these orthopedic surgeries and not PRP? Your guess is as good as mine.
The upshot? Modern orthopedic surgery hasn’t done enough research to support that most of it’s procedures are effective. The research on PRP is actually better or equal in many instances. So why the double standard? My guess is institutional momentum. It’s time to end that orthodoxy…
________________________________________________
References:
(1) Price DD1, Finniss DG, Benedetti F. A comprehensive review of the placebo effect: recent advances and current thought. Annu Rev Psychol. 2008;59:565-90. https://www.ncbi.nlm.nih.gov/pubmed/17550344
(2) Wartolowska K, Judge A, Hopewell S, et al. Use of placebo controls in the evaluation of surgery: systematic review. BMJ. 2014;348:g3253. Published 2014 May 21. doi: 10.1136/bmj.g3253
(3) Louw A, Diener I, Fernández-de-Las-Peñas C, Puentedura EJ. Sham Surgery in Orthopedics: A Systematic Review of the Literature. Pain Med. 2017 Apr 1;18(4):736-750. doi: 10.1093/pm/pnw164.
(4) Moseley JB, O’Malley K, Petersen NJ, Menke TJ, Brody BA, Kuykendall DH, Hollingsworth JC, Ashton CM, Wray NP. A controlled trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med. 2002 Jul 11;347(2):81-8. https://www.ncbi.nlm.nih.gov/pubmed/12110735
(5) Sihvonen R, Paavola M, Malmivaara A, Itälä A, Joukainen A, Nurmi H, Kalske J, Järvinen TL; Finnish Degenerative Meniscal Lesion Study (FIDELITY) Group. Arthroscopic partial meniscectomy versus sham surgery for a degenerative meniscal tear. N Engl J Med. 2013 Dec 26;369(26):2515-24. doi: 10.1056/NEJMoa1305189.
(6) Khatri C, Ahmed I, Parsons H, Smith NA, Lawrence TM, Modi CS, Drew SJ, Bhabra G, Parsons NR, Underwood M, Metcalfe AJ. The Natural History of Full-Thickness Rotator Cuff Tears in Randomized Controlled Trials: A Systematic Review and Meta-analysis. Am J Sports Med. 2019 Jun;47(7):1734-1743. doi: 10.1177/0363546518780694.
(7) Okamura K, Kobayashi T, Yamamoto A, Shitara H, Osawa T, Ichinose T, Takagishi K. Shoulder pain and intra-articular interleukin-8 levels in patients with rotator cuff tears. Int J Rheum Dis. 2017 Feb;20(2):177-181. doi: 10.1111/1756-185X.12581
(8) Kukkonen J, Joukainen A, Lehtinen J, Mattila KT, Tuominen EK, Kauko T, Aärimaa V. Treatment of non-traumatic rotator cuff tears: A randomised controlled trial with one-year clinical results. Bone Joint J. 2014 Jan;96-B(1):75-81. doi: 10.1302/0301-620X.96B1.32168.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.