Understanding Shoulder Labral Tears and Recovery Options
This location is for evaluation appointments only.
A shoulder labral tear occurs when the labrum, a ring of fibrocartilage that helps stabilize and cushion the shoulder joint, is damaged. This injury may result from acute trauma, repetitive motion, or age-related wear. Symptoms frequently include discomfort, instability, and limited shoulder function.
Initial treatment typically concentrates on managing discomfort; however, this approach may fail to address contributing issues such as rotator cuff injuries or joint degeneration. In more severe cases, surgery may be recommended to restore stability, although surgical procedures carry potential risks such as infection, extended recovery time, and variable outcomes.
Physicians in the licensed Regenexx network perform outpatient procedures using Regenexx injectates as a non-surgical option. These image-guided treatments utilize interventional orthobiologics to support the body’s natural healing process. This approach provides a less invasive alternative that may help reduce the need for surgery and long-term use of prescription medications.
Shoulder Labrum Anatomy and Functions
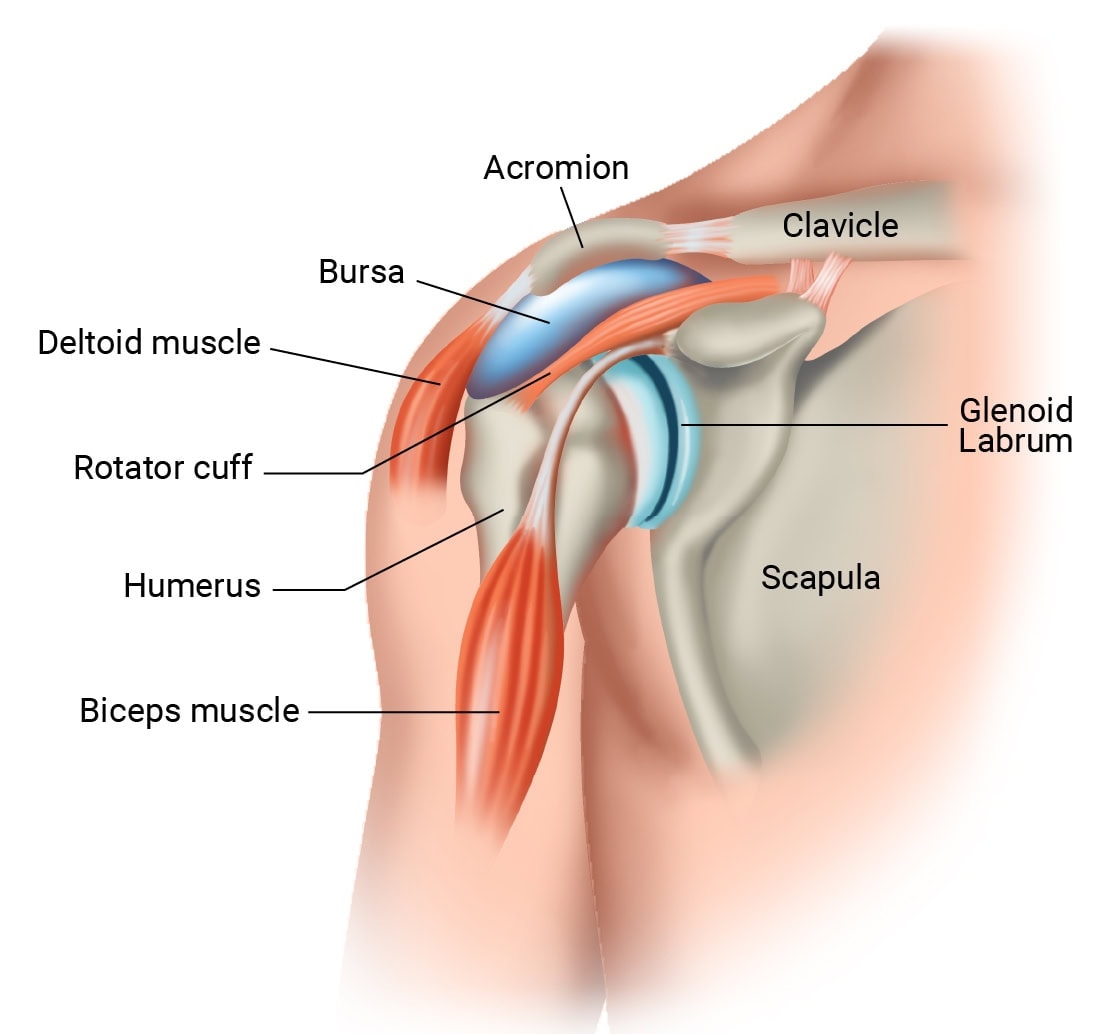
The shoulder joint connects three main bones:
- Humerus: the upper arm bone
- Scapula: the shoulder blade
- Clavicle: the collarbone
The shoulder’s primary joint, the glenohumeral joint, is a ball-and-socket connection where the head of the upper arm bone (the “ball”) fits into the shallow glenoid socket of the shoulder blade. This design enables a wide range of arm movement but is naturally less stable because of the socket’s shallow depth.
Encircling the edge of the glenoid is the labrum, a sturdy ring of cartilage that deepens the socket. Functioning like a bumper, the labrum helps hold the humeral head securely, improving joint stability while maintaining the shoulder’s flexibility.
What Is a Labral Tear in the Shoulder?
A labral tear involves damage to the cartilage lining the shoulder joint. This occurs when the collagen fibers of the labrum are stressed through repeated motion or sudden injury. Labral tears are fairly common among active individuals and may become more likely with age.
These tears can be classified as acute or traumatic. Acute tears usually arise from a single, high-force event that stretches or damages the labral tissue. Research has shown that some labral tears can exist without noticeable symptoms; for instance, MRI scans have revealed labral injuries in a significant portion of asymptomatic athletes.
Labral tears may also coincide with other shoulder injuries. Common scenarios include:
- Dislocations: Complete displacement of the upper arm bone from the shoulder socket.
- Subluxations: Partial dislocations where bones shift out of alignment but remain partially in place.
When the shoulder bones move abnormally, additional stress is placed on the labrum, which can worsen existing tears.
Types of Labral Tears in the Shoulder
Labral tears are often classified by location and mechanism:
- Anterior Labral Tear (Bankart Lesion): Occurs at the front of the labrum, often linked to dislocations or repeated overhead activity.
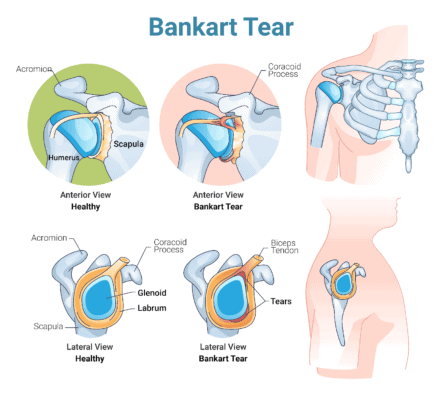
- Posterior Labral Tear (Reverse Bankart Lesion): Affects the back of the labrum, typically caused by repeated compression or rotational stress. Less common than other types.
- SLAP Tear (Superior Labrum, Anterior to Posterior): Involves the top portion of the labrum where the biceps tendon attaches, potentially causing pain, instability, and limited function.

- Degenerative Labral Tear: Develops gradually due to age-related wear and is often associated with osteoarthritis.
Labral Tears Symptoms
Some labral tears may remain asymptomatic. Studies have found that a significant number of individuals may have labral irregularities without experiencing pain or functional issues. When symptoms do occur, they can include:
Pain and Swelling
Damage to the labrum can produce deep or localized shoulder pain. The body’s natural inflammatory response may cause swelling, which is often more intense after acute injury. Mild inflammation may persist long-term in some cases.
Popping, Locking, or Grinding
Shoulder injuries may produce a popping sensation at the time of trauma. Subsequent movements can lead to clicking, grinding, or temporary joint locking. Uneven surfaces caused by a tear can produce audible sounds or vibrations, sometimes without pain.
Reduced Range of Motion
Labral damage may restrict shoulder mobility. Pain, swelling, and interference from torn tissue can limit smooth movement, and prolonged reduced use can lead to stiffness in surrounding muscles.
Shoulder Dislocation

Labral tears can weaken shoulder stability, increasing the risk of dislocations. Recurrent dislocations may further damage the labrum, potentially creating a cycle of instability that sometimes requires surgical intervention.
Weakness and Instability
A torn labrum can make the shoulder feel unstable during activities such as lifting or throwing. This “giving way” sensation is due to the labrum’s diminished role in stabilizing the joint.
Difficulty Sleeping on the Affected Side
Pain or discomfort can make it challenging to sleep on the injured shoulder. Pressure on the joint can worsen inflammation and disturb sleep.
Investigating the Causes and Risk Factors
Labral tears in the shoulder are typically classified into two main types:
- Acute labral tears: Usually caused by sudden trauma, such as a fall onto an outstretched hand or a direct impact to the shoulder.
- Degenerative labral tears: Develop gradually over time due to age-related changes or repeated stress on the shoulder joint.
Contributing Factors and Risk Factors
- Repetitive overhead activities: Frequent motions, such as throwing or lifting, can cause microtrauma that gradually leads to labral tears.
- Postural imbalances: Slouching or forward head posture increases stress on the shoulder joint.
- Age-related degeneration: Natural wear of cartilage and soft tissues over time may result in tearing even without a specific injury.
- Glenoid (shoulder socket) irregularities: Structural variations in the socket can place additional strain on the labrum.
- Connective tissue conditions: Inherited disorders, such as Ehlers-Danlos syndrome, cause joint laxity and increase friction within the joint.
- Scapular dyskinesis: Abnormal movement of the shoulder blade disrupts joint alignment and can accelerate labral wear.
- Prolonged or improper crutch use: Extended or incorrect use of crutches may place ongoing strain on the shoulder.
- History of shoulder surgery: Scar tissue or altered joint mechanics from previous procedures may raise the risk of tears.
- Shoulder-intensive activities: Sports or occupations that involve frequent shoulder use, such as swimming or gymnastics, can increase wear on the labrum.
Diagnosing a Labral Tear in the Shoulder
Diagnosis typically involves a combination of methods:
- Medical History and Symptom Review: Consideration of prior dislocations, surgeries, or genetic conditions.
- Physical Examination: Assessment of pain, instability, and joint mechanics through specific shoulder movements.
- Imaging: MRI or ultrasound provides detailed visualization of the labrum, while X-rays help rule out bone-related issues.
Conventional Treatment Options
Conventional treatment approaches are intended to help reduce symptom severity and support improved shoulder function. These may include both non-surgical and surgical options.
Non-Surgical Treatment Options
Treatment aims to relieve symptoms and restore shoulder function. Options include both non-surgical and surgical approaches.
Non-Surgical Management
Non-invasive strategies are usually the first step:
- Activity Modification: Rest and temporary adjustments reduce strain and allow healing.
- Physical Therapy: Targeted exercises improve stability, strengthen muscles, and enhance range of motion.
Surgical Interventions
Surgery may be needed for severe tears or persistent dysfunction. Procedures are designed to repair structural damage and improve stability:
- Arthroscopic Repair: Minimally invasive approach using small incisions and a camera to guide repair.
- Labrum Reattachment: Larger procedures use anchors to secure the torn labrum to bone.
Any surgical procedure carries potential risks, including the possibility of infection and an extended recovery period. One study also identified specific complications related to labral repair, such as:
- Anchor failure: The small devices used to secure tissue can fail if improperly placed or due to material fatigue over time.
- Chondrolysis: A rare but serious complication characterized by rapid cartilage loss, leading to decreased joint space.
Recovery from labral surgery may require several months of restricted activity to allow proper healing and restore shoulder function.
How Successful Is Shoulder Labrum Repair Surgery?
Surgical repair for a labral tear often involves procedures such as repositioning the biceps tendon to stabilize the shoulder joint. While surgery can provide benefits in select cases, it carries inherent risks and typically requires a prolonged recovery period that includes structured physical therapy.
In some instances, surgical intervention may not fully restore shoulder stability, which can leave the joint susceptible to future injuries. Consulting with a physician to review all available treatment options is essential in determining the most appropriate care plan.
Can Recovery from Tears Be Accelerated Without Surgery?
Although labral repair surgery can provide relief for some patients, results are not always predictable. Research published in 2021 highlighted post-surgical complications such as subluxation, full dislocation, and persistent instability, with some cases requiring additional revision procedures. As with any invasive treatment, risks such as infection and extended rehabilitation periods should be considered.
Not every labral tear necessitates surgery. Many individuals experience improved shoulder function through non-surgical strategies, avoiding the potential complications and downtime associated with invasive procedures.
The Regenexx approach offers a non-surgical alternative, using personalized interventional orthobiologics—including platelet-rich plasma (PRP) and bone marrow concentrate (BMC)—to stimulate the body’s natural healing mechanisms and support recovery.
Pain Doctors Medical: Supporting Shoulder Function Recovery
The Regenexx approach at Pain Doctors Medical utilizes interventional orthobiologics to support the body’s natural healing process. Procedures using Regenexx injectates may serve as an alternative for individuals seeking to avoid surgery, extended recovery, or long-term use of prescription pain medications.
The classification and severity of the labral tear help the physician determine whether this approach may be suitable. A thorough evaluation by a physician in the licensed Regenexx network is the first step.
Customized treatment plans may include one or more of the orthobiologics below.
- Regenexx SD Injectate: Procedures using Regenexx SD injectate follow a proprietary protocol involving Bone Marrow Concentrate (BMC). BMC contains the patient’s own cellular healing agents. The lab processing routinely achieves a significantly higher concentration of cells compared to typical non-Regenexx methods.
- Regenexx SCP Injectate: This concentrated formulation of platelet-rich plasma (PRP) is created by drawing blood and isolating growth factors. The solution is delivered with imaging guidance for accuracy. The SCP injectate contains a higher concentration of growth factors than typical PRP.
- Regenexx PL Injectate: Regenexx PL injectate delivers a fast-acting, highly concentrated release of growth factors. This specialized derivative of PRP is often used in combination with other orthobiologics, such as PRP and BMC, as part of comprehensive treatment strategies.
Help Improve Shoulder Function Without Surgery
Shoulder labrum tears can affect mobility and make daily activities difficult or painful. For individuals who have not found relief with medication, surgery is not the only option.
Procedures using Regenexx injectates at Pain Doctors Medical in New Jersey utilize interventional orthobiologics to support the body’s natural ability to address tissue injury. This non-surgical approach may help improve shoulder function, mobility, and joint stability without the need for invasive intervention.
75 Smith Street
Perth Amboy, NJ 08861
Request an Appointment
Call to Schedule Schedule OnlineClinic Hours
| Sunday | Closed |
| Monday | 9AM–5PM |
| Tuesday | 9AM–5PM |
| Wednesday | 9AM–5PM |
| Thursday | 9AM–5PM |
| Friday | 9AM–5PM |
| Saturday | Closed |

Treat Labral Tears Without Surgery
Regenexx procedures are non-surgical treatments that use your body’s own healing agents to treat shoulder labral tears. Our patients benefit from reduced pain and improved function, helping them avoid shoulder surgery.
Regenexx Procedures for Labral Tears
Regenexx’s percutaneous labralplasty is a nonsurgical procedure that uses precise imaging guidance and your own healing cells to promote natural healing. Regenexx procedures can be a better alternative for people looking to avoid surgery, lengthy recovery, and overuse of prescription pain medication. They use either platelet-rich plasma or bone marrow concentrate (which contains stem cells).
The nature and severity of your labral tear (classification type) generally determines if the treatment is right for you. An evaluation by a Regenexx physician is the first step.
Find a Location
Find a physician in licensed Regenexx network.
Labral Tear Repair Patient Stories
I tell people about it all the time, and they find it so hard to grasp…100% and no scars, no downtime….I am so happy with my results and just wanted to say THANKS once again.”
Pilates lover with an active lifestyle – Full patient story
Number 8 [at 3 minutes and 35 seconds] is Matt scoring the winning goal for Penn State lead over Cornell. He had 2 great goals! THANK YOU…he feels great:)”
Mother of a college athlete – Full patient story
Note: Like all medical procedures, Regenexx procedures have a success and failure rate. Not all patients will experience the same results.
Webinar: Alternatives to Shoulder Labrum Surgery
Learn the latest about regenerative medicine, and how Regenexx procedures can treat your shoulder labrum injury.
Patient FAQs
Yes, not everyone experiences pain when their labrum is torn. In 2016, a study performed MRIs on patients without shoulder pain who were 45-60 years old, a staggering 55-72% of these people had labral tears. 5
Yes. When the tear is in the upper part of the labrum, the area where the biceps tendon attaches to the lap of the socket is also commonly torn. When this happens, it’s called a SLAP tear (Superior Labral Tear from Anterior to Posterior).
Get started to see if you are a Regenexx candidate
To talk one-on-one with one of our team members about how the Regenexx approach may be able to help your orthopedic pain or injury, please complete the form below and we will be in touch with you within the next business day.
References
1. Clavert P. Glenoid labrum pathology. Orthop Traumatol Surg Res. 2015 Feb;101(1 Suppl):S19-24. doi: 10.1016/j.otsr.2014.06.028. Epub 2015 Jan 14. PMID: 25596985.
2. Van Blarcum GS, Svoboda SJ. Glenohumeral Instability Related to Special Conditions: SLAP Tears, Pan-labral Tears, and Multidirectional Instability. Sports Med Arthrosc Rev. 2017 Sep;25(3):e12-e17. doi: 10.1097/JSA.0000000000000153. PMID: 28777213.
3. Schrøder CP, Skare Ø, Reikerås O, Mowinckel P, Brox JI. Sham surgery versus labral repair or biceps tenodesis for type II SLAP lesions of the shoulder: a three-armed randomised clinical trial. Br J Sports Med. 2017 Dec;51(24):1759-1766. doi: 10.1136/bjsports-2016-097098. Epub 2017 May 11. PMID: 28495804; PMCID: PMC5754846.
4. Schwartzberg R, Reuss BL, Burkhart BG, Butterfield M, Wu JY, McLean KW. High Prevalence of Superior Labral Tears Diagnosed by MRI in Middle-Aged Patients With Asymptomatic Shoulders. Orthop J Sports Med. 2016 Jan 5;4(1):2325967115623212. doi: 10.1177/2325967115623212. PMID: 26779556; PMCID: PMC4710128.
5. Cruz-Ferreira E, Abadie P, Godenèche A, Mansat P, Clavert P, Flurin P; French Arthroscopy Society. Posterior shoulder instability: Prospective non-randomised comparison of operative and non-operative treatment in 51 patients. Orthop Traumatol Surg Res. 2017 Dec;103(8S):S185-S188. doi: 10.1016/j.otsr.2017.08.004. Epub 2017 Sep 2. PMID: 28873349.
- Hip Labrum Surgery Mania
- Torn Hip Labrum and Hip Osteoarthritis
